How Often Should Providers Verify a Patient's Medicaid Eligibility
Medicaid is a joint federal and state program that together with the Childrens Health Insurance Program CHIP provides health coverage to over 725 million Americans including children pregnant women parents seniors and individuals with disabilities. Providers should also periodically review the beneficiarys eligibility information as long as the patient is receiving services from your agency.
Who are the experts.

. Providers should note that the article in the April 1991 Provider Update discussion Medicaid of Louisianas policy on requests for adjustment of cost per discharge limits contained some errors. At the time of the patients annual wellness checkup b. By ensuring access to employer-sponsored health insurance people who are eligible for HIPP can receive services that are not normally covered through Medicaid.
These services are provided through a large network of health care. Use the eligibility response to prepare accurate Medicare claims determine patient liability or check eligibility for specific services. Find your MACs website to register for your MACs portal.
Some providers have noted that a recipient may have a valid Medicaid or Health Choice ID card but not be listed as eligible in NCTracks. Providers servicing displaced Florida Medicaid recipients who do not have an active Florida Medicaid Provider ID will need to. A primary care provider may be interested only in whether or not the insurance is in effect at the time of.
Enrollee whose eligibility has been delayed. There are many missed opportunities to secure income and reduce staff time when patient eligibility is not verified at the time of check in. Providers can benefit from this program by receiving a higher payment from the employer-sponsored health insurance carrier than from Medicaid.
Solutions for Chapter 10 Problem 1Q. With each visit to the provider. Convert the target amount for current period to a per diem amount by multiplying the target for the cost.
Medicaid eligibility verification process should ideally start before offering the clinical services and be undertaken with utmost care. HIPP helps people who might otherwise be uninsured. Get solutions Get solutions Get solutions done loading Looking for the textbook.
Like other care providers those reimbursed by Medicaid have a hard time connecting with patients beyond the traditional office visit. The following steps can ensure the reduction of eligibility-based denials for any healthcare provider billing team. CMS offers an X12 270271 Eligibility System HETS 270271.
NCTracks is now offering a new service for providers to verify recipient eligibility. Medicaid is the single largest source of health coverage in the United. This table depicts key elements of states proposed approach to verifying the factors of eligibility for coverage in Medicaid and Childrens Health Insurance Program CHIP.
Prior to submission of the home health request for anticipated payment RAP. Verify eligibility and coverage for the presented medicaid number whether the medicaid card is valid or if a managed medicaid insurer has been selected. This can often be accomplished by checking the website of the insurance carrier or calling a representative of the insurance carrier.
L0 104 What steps should be taken to verify a patients Medicaid eligibility. It is the providers obligation to verify the patients Medicaid eligibility. For being eligible for medical aid one must meet the requirements for an eligibility group that thestate covers.
We review their content and use your feedback to keep the quality high. Experts are tested by Chegg as specialists in their subject area. When the patient notifies you of any changes in Medicaid coverage d.
The HIPAA Eligibility Transaction System HETS is intended to allow the release of eligibility data to Medicare Providers Suppliers or their authorized billing agents for the purpose of preparing an accurate Medicare claim determining Beneficiary liability or determining eligibility for specific. New Yorks Medicaid program provides comprehensive health coverage to more than 73 million lower-income New Yorkers as of December 2021 Medicaid pays for a wide-range of services depending on your age financial circumstances family situation or living arrangements. Doctors are less inclined to accept Medicaid patients to begin with especially in states like New Jersey and patients often spend less time overall engaging in face-to-face interaction with their care providers.
First a provider can check a recipients Medicaid eligibility on NCTracks and if not there can call the NCTracks Call Center. It is essential that every physician practice verify the insurance eligibility and benefits of patients before services are provided. How frequently should a patients Medicaid eligibility be verified.
Items c and d read incorrect as follows. This electronic verification process will provide date specific eligibility which will help reduce claim denials related to eligibility. The Affordable Care Act and accompanying federal regulations have established a modernized data driven approach to verification of financial and non-financial information needed to.
On a monthly basis c. The AVRS requires the use of a nine-digit active Florida Medicaid provider identification ID number to verify recipient eligibility. Virginia VA Medicaid Eligibility.
What steps should be taken to verify a patients Medicaid eligibility. In addition you must also be pregnant a parent or caretaker living in a nursing facility disabled or over age 65. A Medicare beneficiarys eligibility should be checked at a minimum.
Asking the right questions to the patient by the front. Some practice management systems and clearinghouses are also capable of checking patient eligibility. MEVS is available 24 hours a day 7 days a week except for a short maintenance window each week.
Upon admission to your agency. Training staff to complete this task can help boost revenue at time of service and save time on. Answer to L0 104 What steps should be taken to verify a patients M.
MAC Online Provider Portal Each MAC offers its own Medicare online provider portal so you can access information anytime. You may qualify for Medicaid benefits in Virginia if you are a state resident with little to no income. Providers who have rendered care for a period of delayed eligibility will be notified by a copy of a letter from the local department of social services.
It can help to eliminate Medicaid fraud.
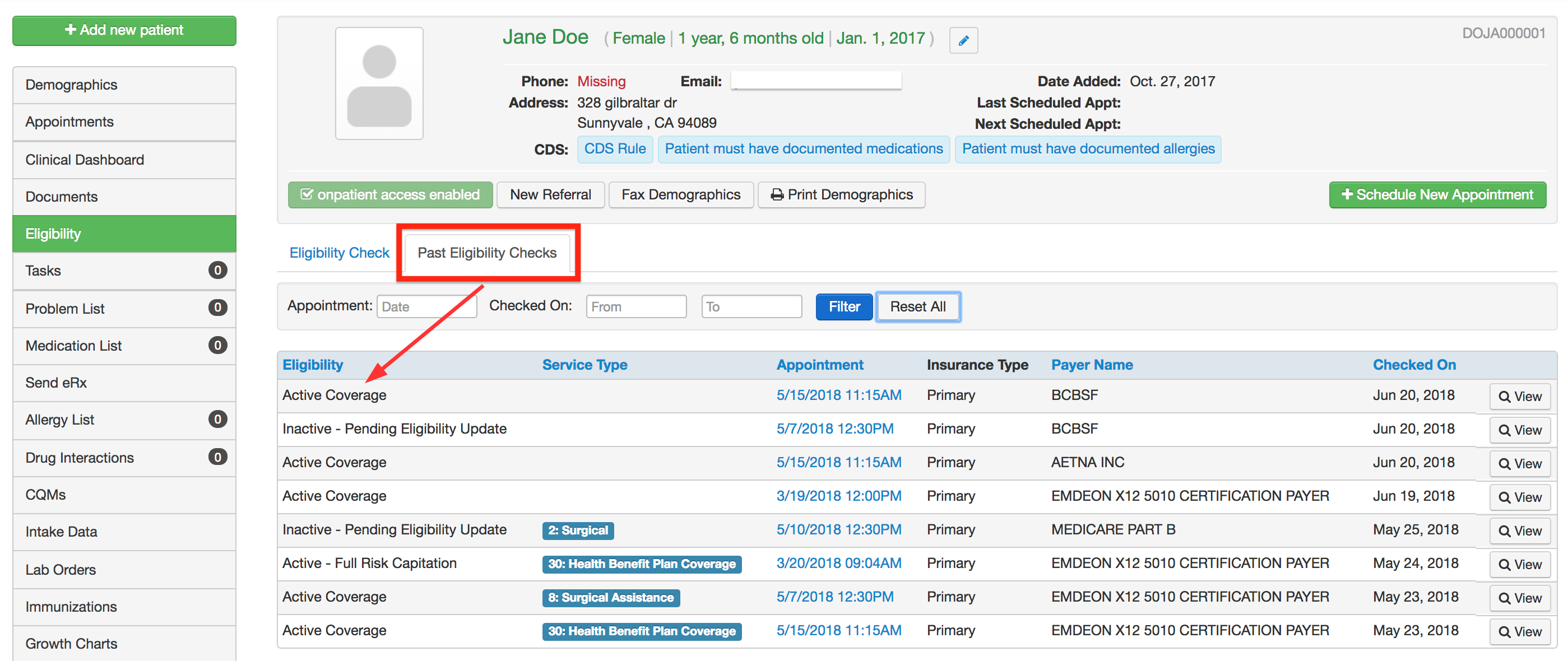
What Is Real Time Eligibility Patient Eligibility Verification

3 Ways To Verify Patient Eligibility Eclaimstatus

Hrsa Uninsured Covid 19 Program How To Verify Patient Eligibility
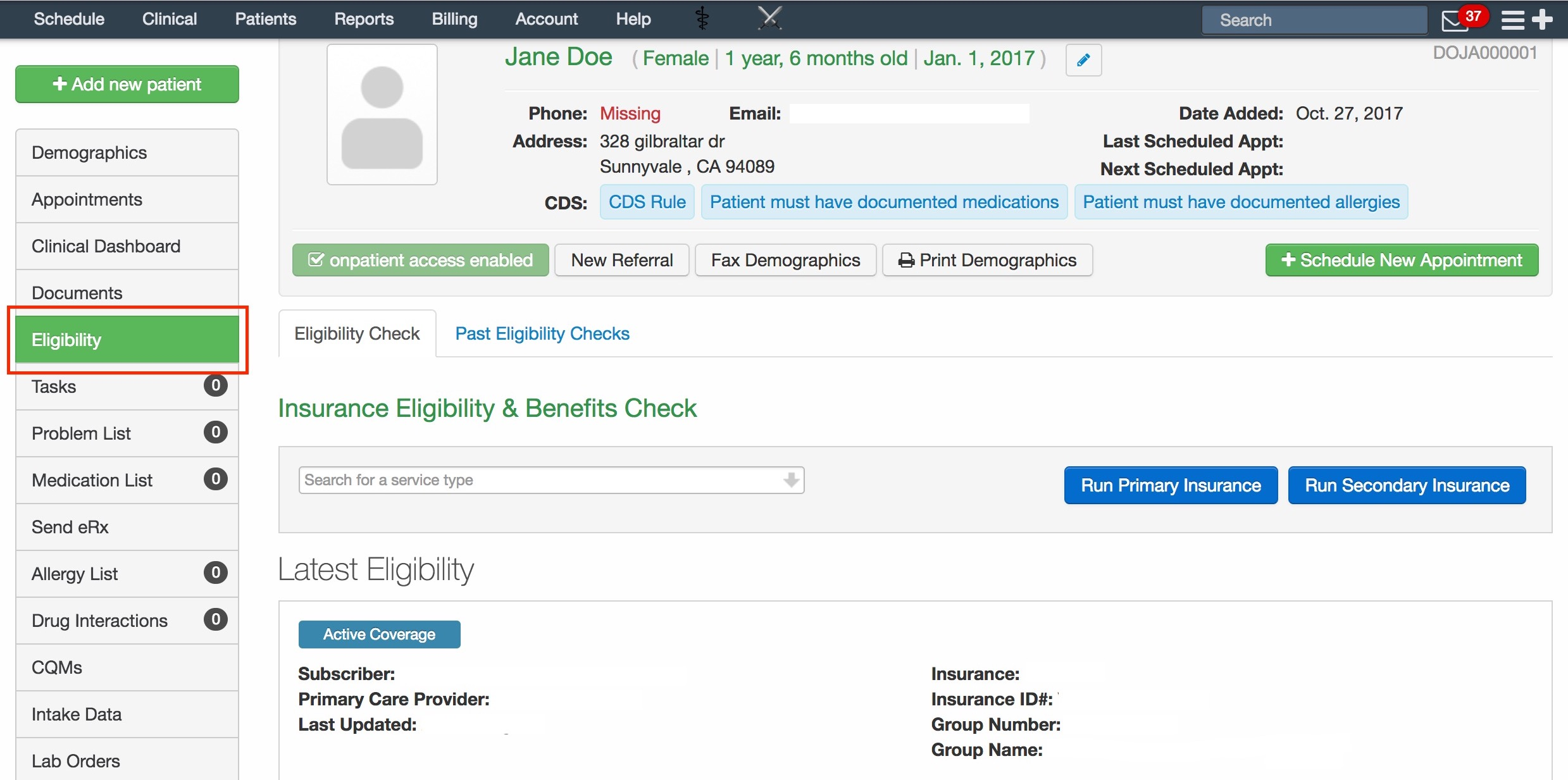
What Is Real Time Eligibility Patient Eligibility Verification

Step Two Verify Patient Eligibility

Prepared By Medwave Billing Credentialing Ppt Download

Patient Eligibility Verification Best Practices The Top 6 Tips
5 Insurance Eligibility Verification Steps For Every Practice

Verify Patients Insurance Eligibility Coverage Before Office Visits The Rheumatologist

What Is Real Time Eligibility Patient Eligibility Verification

What Steps Should Be Taken To Verify A Patient Medicaid Eligibility Eclaimstatus

How To Verify Patient Insurance In Three Easy Steps Webpt

Insurance Eligibility Verification Process In Healthcare Capminds Blog

Patient Eligibility Verification Insurance Eligibility Verification

Understanding Eligibility 5 Questions Answered
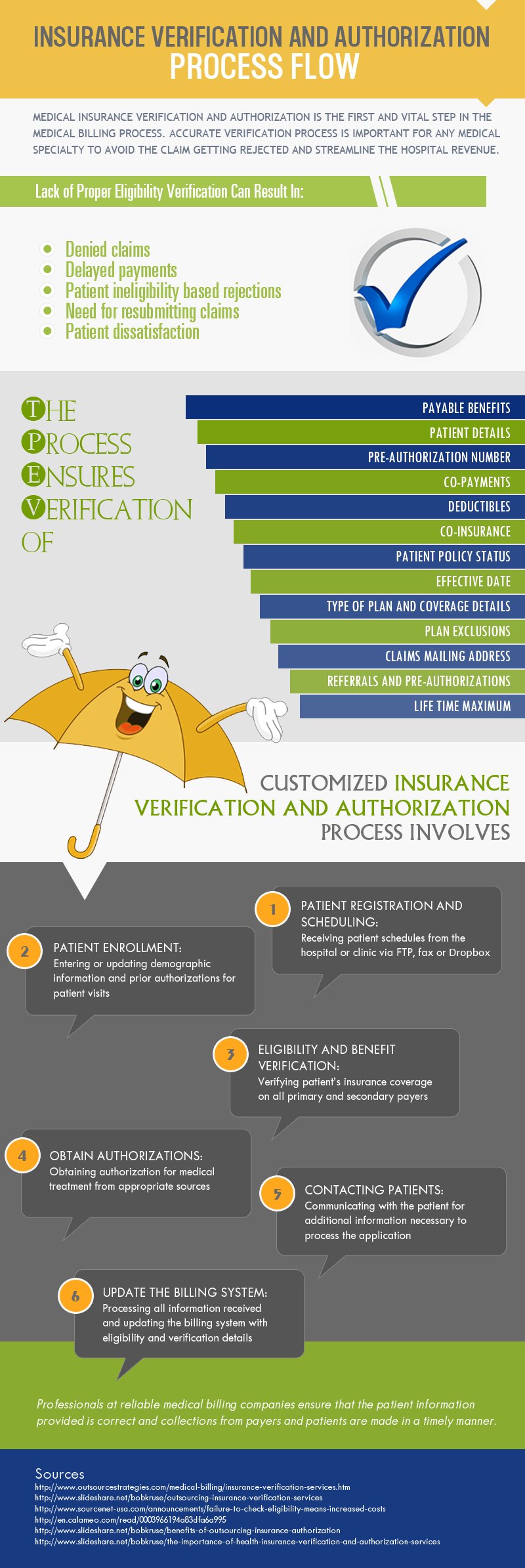
Insurance Authorization Service Insurance Authorization Company

The Importance Of Eligibility And Benefits Verification Drcatalyst



Comments
Post a Comment